Written by Brandon Okey. Mina Draskovic, B.Psy., reviewed this content for accuracy.
Alcohol, a powerful depressant, can severely affect mental health when consumed heavily and regularly. It alters the brain’s chemistry, leading to mood instability, depression, anxiety, and other mental disorders.
Mental health issues can also cause you to be more susceptible to alcohol abuse. Researchers at the University of Liverpool have shown that people with mental disorders are twice as likely to report an alcohol use disorder.
If you’re a heavy drinker and struggle with anxiety, depression, or other mental health problems, maybe it’s time to seek help. We understand that the decision to end alcohol dependency can be difficult, but it’s also life-changing.
Our rehab center welcomes anyone who struggles with addiction.
I went to Ardu only for detox (my first treatment ever) and they made it incredibly comfortable for me. The nurses were awesome! They made it so comfortable for me going through something I felt very nervous about with it being my first time. Staff was welcoming to me to join groups but not pushy as I was detoxing…I can greatly thank Ardu for opening the door of sobriety and treatment to me with the utmost comfort and ease.
Many people resort to drinking for temporary relief from stress, but in the long run, alcohol inflicts severe emotional damage. Alcoholism, or alcohol use disorder (AUD), is associated with a wide range of mental health issues.
Here’s what you need to know:
According to the Substance Abuse and Mental Health Services Administration, “people who abuse substances often present with medical conditions in advanced stages or in a medical crisis. Co-occurring mental disorders also are likely to be exacerbated by substance abuse.”
Here are some mental disorders that alcohol may lead to:
Addiction treatment programs involve much more than simply treating the symptoms of alcohol withdrawal. At Ardu, we take care of your physical and mental health equally. Ardu’s mental health treatment programs offer a supportive environment tasked with improving our residents’ lives every day.
A 2002 study revealed that around 37% of people who misuse alcohol or suffer from alcohol dependence have at least one serious mental health disorder. Out of all those diagnosed as mentally ill, 29% of them abuse alcohol or drugs.
The table below shows the prevalence rates of psychiatric disorders among the respondents to the National Comorbidity Survey and the Epidemiologic Catchment Area study who were diagnosed with alcohol abuse or dependence and a comorbid psychiatric disorder.
Comorbid disorder | 1-year rate for alcohol abuse | 1-year rate for alcoholism |
Major depressive disorder | 11.3 | 27.2 |
Bipolar disorder | 0.3 | 1.9 |
Generalized anxiety disorder (GAD) | 1.4 | 11.6 |
Panic disorder | 1.3 | 3.9 |
PTSD | 5.6 | 7.7 |
As you can see, people struggling with alcohol dependence had higher rates of comorbid psychiatric disorders compared to those with abuse. The rates for mental disorders were higher among individuals with alcoholism compared to alcohol abuse. These findings suggest a strong association between alcohol use disorders and other psychiatric conditions, emphasizing the need for integrated treatment approaches for people with comorbid disorders.
Our dual diagnosis program recognizes the complex interplay between addiction and mental health. We provide a personalized integrated treatment plan that addresses substance use and psychiatric issues simultaneously.
You don’t have to navigate recovery alone. Contact Ardu and let’s discuss your treatment options.
Alcohol may spur a fun buzz temporarily, but heavy, consistent drinking can have some severe psychological impacts. It sabotages mental health, both through mood and behavioral volatility. In the short term, booze impairs judgment and lowers inhibitions, leading to regrettable behaviors. Over time, it restructures the neural pathways affecting emotion regulation and impulse control. The more and longer you drink, the more cognition and sanity erode.
Here’s how alcohol may affect you psychologically:
If you think this is bad, wait until you hear about the long-term effects of alcohol on your mental health.
Alcohol doesn’t just impact your moods and thoughts. It can change your behavior, too. It all comes down to the way booze affects the brain—and not in a good way.
You can find the caring treatment you need for your problems with alcohol and mental health issues. Our team of compassionate professionals at the depression treatment center understand the multi-faceted nature of these conditions. You can benefit from our holistic detox where we address the root causes of mood disorders.
Alcohol does a number on your brain. It induces structural changes while also interfering with the brain’s intricate chemical signaling processes. While some of these effects are acute (they go away when the body gets rid of toxins), others can be longer-lasting. Alcohol may cause physical and functional brain damage that can impair your cognitive abilities and severely change your emotional state.
Initially, booze has sedating effects and provides a nice mood lift. The more you drink, the more alcohol suppresses the chemicals in your brain—the neurotransmitters responsible for emotions. Over time, chronic alcohol abuse causes structural changes to the frontal lobe and the limbic system. These brain regions are integral to emotional processing, cognition, reasoning, and impulse control.
Neurotransmitters are chemical messengers that enable communication between neurons, regulating mood, cognition, movement, and many other critical functions.
…minimal alcohol intake will enter the brain and target GABAA receptors, causing a cascade of regulatory events, potentially leading to behavioral changes. When consumption becomes chronic, or during binge drinking episodes, the impact of alcohol on the brain is even more profound… (Dharavath, et. al.)
Alcohol has negative effects on several neurotransmitters that are vital for maintaining mental health. In particular, it disrupts dopamine, serotonin, and GABA.
Dopamine regulates motivation, pleasure, and motor functions. After a drink or two, alcohol provides a temporary dopamine surge, creating a “high.” In the long run, you start needing more and more to capture that pleasurable dopamine rush, leading to the suppression of the dopaminergic system.
Dopamine-containing neurons in the NAc [nucleus accumbens] are activated by motivational stimuli, which encourage a person to perform or repeat a behavior. Even low alcohol doses can increase dopamine release in part of the NAc. This dopamine release may contribute to the rewarding effects of alcohol and may thereby play a role in promoting alcohol consumption. (Di Chiara, M. D.)
This spiral exacerbates addiction and leads to a decline in mental health. A dopamine deficiency can lead to anhedonia, apathy, and clinical depression, robbing you of the ability to feel motivation or pleasure.
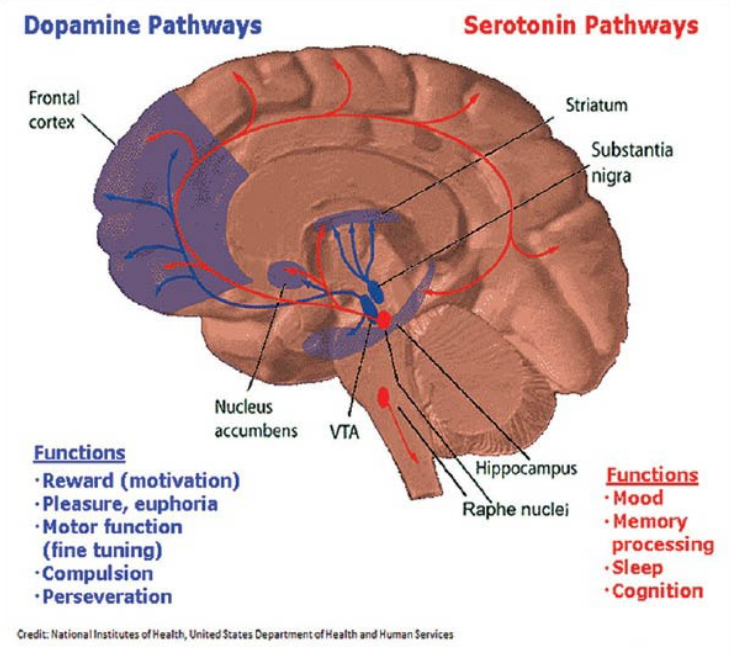
Serotonin is a neurotransmitter critical for regulating mood, sleep cycles, cognition, appetite, and impulsivity. Optimal serotonin levels promote stable mood, calmness, focus, and emotional control. When you don’t have enough of it, you may be at risk of developing depression, anxiety disorders, aggression issues, and low tolerance for stress.
Alcohol provides an immediate, artificial serotonin boost, acting as an antidepressant, but chronic heavy alcohol use depletes serotonin by interfering with production and depleting reserves. This leads to anxiety, irritability, poor sleep quality, cloudy thinking, and clinical mood disorders common among those with alcohol use disorders (AUD).
A 2014 study found that during withdrawal, the nucleus accumbens region releases less serotonin, contributing to negative mood states. You drink to temporarily restore serotonin levels and alleviate withdrawal symptoms, further perpetuating the addiction cycle.
GABA is the brain’s primary inhibitory neurotransmitter. It regulates nervous system activity by reducing neuron excitability. Initially, alcohol enhances GABA release, providing short-term relief from anxiety and psychological distress.
In people addicted to alcohol, GABA receptor density is depleted, and the signaling between GABA and its receptors is disrupted. This reduces GABA’s calming ability, increasing your susceptibility to stress and emotions.
The effects of chronic ethanol administration are influenced by adaptations in GABAA receptor function, expression, trafficking, and subcellular localization that contribute to ethanol tolerance, dependence, and withdrawal hyperexcitability. (Kumar, et. al.)
Decreases in GABA inhibition are linked to an increased risk for anxiety, agitation, insomnia, and even alcohol withdrawal syndrome. This is why chronic alcohol use so often goes hand in hand with mood disorders as well as addiction and abuse.
The good news is, when you stop drinking, your brain experiences recovery, as the levels of GABA and other neurotransmitters return to balance. Ardu is here to facilitate your restoration of health.
You can expect the highest quality care at Ardu, with our success rooted in compassionate support of each person’s unique mental health needs and recovery goals. Holistic approaches such as yoga and meditation can help curb anxious thoughts.
Structural degradation in areas integral to emotional stability, self-control, and coping capacities pave the way to psychiatric issues prevalent among those with alcohol use disorders.
Research shows that excessive alcohol can physically change your brain. Alcohol can shrink the gray and white matter over time, affecting areas such as the prefrontal cortex and hippocampus. As brain volume shrinks, important neurotransmitters are damaged and imbalanced.
Alcohol affects two important brain regions: the frontal lobe and the limbic system.
Studies involving human subjects with chronic alcohol use have demonstrated reduced hippocampal volume, postmortem evidence of prior neuronal loss, and severely reduced hippocampal activity, including reductions in blood flow. (Staples and Mandyam)
These changes can have long-term consequences on cognitive abilities and emotional regulation, possibly leading to or worsening mental health issues such as anxiety and mood disorders.
Through impacts on these intricate neuro-chemical interactions and pathways, excessive drinking restructures the brain in ways known to agitate many psychiatric illnesses. The good news is, when you stop drinking, your brain recovers: the levels of neurotransmitters return to balance, new neurons can grow, and your mental health may improve with sustained sobriety.
The recovery process begins with alcohol detox. This is an essential first step, where we safely and comfortably help your body cleanse from alcohol toxins and bring harmony to your brain’s chemical wiring. The medical professionals at our detox center closely monitor your progress to ensure a smooth and safe detox experience.
Alcoholism is considered a mental disease by some people. The disease model of addiction suggests that alcoholism is not as simple as moral failure or a lack of self-control but is also based on some fundamental changes in brain structure.
According to the National Institute for Alcohol Abuse and Alcoholism, AUD is a chronic relapsing brain disease characterized by an impaired ability to stop or control alcohol use despite adverse social, occupational, or health consequences. It involves both a physical dependency on alcohol, which can lead to withdrawal symptoms when not consumed, and a mental obsession with alcohol, which affects the person’s ability to control their consumption.
Our goal is to treat alcohol addiction and co-occurring mental health disorders simultaneously. We want you to regain control over your life, help you treat cravings and withdrawal symptoms, and prevent chronic relapse.
Don’t feel bad if you stumble and fall back to your bad habits. Relapse is an unavoidable part of recovery. Our evidence-based relapse prevention treatment aids in identifying triggers, developing coping strategies, and building a supportive community to minimize the occurrence of relapses.
Do you want to eliminate alcohol from your life and recover your mental health? We are here for you.
Our dual diagnosis treatment has skilled healthcare providers with extensive experience in treating alcohol addiction related to other mental and physical health disorders. Ardu can help you cope with mental illnesses that complicate the process of recovering from addiction.
We offer a range of treatment options to help you overcome addiction and address co-occurring mental health issues.
Our cognitive behavioral therapy can help you build coping strategies to manage destructive thought patterns fueling mood instability and addictive impulses. Our team managing self-compassion techniques can teach you how to eliminate the extreme self-criticism that drives anxiety and depression.
Integrate these complementary modalities and ease the psychological, neurological, and spiritual healing required to overcome addiction’s damage.
In addition to treatment for alcoholism, we also offer treatment for other substance use disorders. Our addiction treatment services include EMDR therapy, experiential therapy, contingency management, and more. Contact us to get informed and start your sobriety journey.

Brandon Okey is the co-founder of Ardu Recovery Center and is dedicated to empowering people on their journey to sobriety.
Alcohol is highly addictive, with about 20% of Americans with an alcohol or substance use disorder also experiencing anxiety or mood disorders. Research has shown that alcohol use disorders have a lifetime prevalence of 12.6% to 27.5% for alcohol abuse or dependence. The addictive nature of alcohol is further compounded by its impact on the brain, leading to physical dependency and the development of comorbidities with other substance use and psychiatric disorders.
Alcohol co-opts the brain’s dopamine reward circuitry (which regulates motivation and decision-making capacities) by over-stimulating it. This reinforces habitual substance-seeking despite escalating negative consequences indicative of progressive use disorders reflecting potential severity levels.
Heavy drinking also disrupts finely-tuned GABA and glutamatergic neurotransmitter systems. This makes you feel agitated when you’re not consuming amounts sufficient to mitigate pounding cravings. This neural adaptation conduits alcohol dependence by shrinking grey matter volume integrity governing behavioral self-regulation.
Holistic, integrated treatment approaches focused on harm reduction help deconstruct addiction’s grip through lifestyle adjustments addressing biopsychosocial well-being.
Alcohol is the depressant of the central nervous system, which makes it a natural depressant. While initially spurring short-term euphoria, drinking regularly progressively depletes vital signaling chemicals and causes depressive effects. Alcohol suppresses neural activity by slowing communication between excitatory neurotransmitters including dopamine, acetylcholine, norepinephrine, and serotonin. These chemical messengers direct motivation, alertness, and mood stability. The eventual atrophy of self-soothing neural frameworks alongside electrolyte loss leaves drinkers ricocheting between negative feelings and manic highs during repeated detox cycles.
For those with underlying psychiatric issues or a history of psychosis, alcohol abuse, even in lower amounts, can dramatically escalate disconnects with reality, also known as psychosis. It can cause hallucinations, delusional disorganization, and irrational thinking because dopamine, GABA, and glutamatergic systems are disrupted.
Binge drinking also spikes cortisol, inducing a distressed neurological state mirroring psychotic disorders. With repeated bouts shrinking the hippocampus and frontal lobe, as well as compromising neurotransmitters, substance-activated rewiring may profoundly rupture cognitive functioning. Approximately half of those struggling with AUD have co-occurring disorders that exacerbate each other’s severity.
Post-intoxication residue includes seesawing neurochemicals and hormones as well as electrolyte crashes. When you drink, alcohol triggers inflammation in the body producing and accumulating toxic waste products and sensitization echoes. This delayed come-down marks the strenuous journey toward renewed stability and well-being. Accepting lingering feelings of weirdness as byproducts of substance-disarrayed systems helps strengthen self-compassion to accelerate healing through balanced self-care approaches.
Alcohol’s oxidative stress and accumulating inflammatory waste products severely accelerate aging. Booze corrodes cell membrane structural integrity, frays protective DNA telomeres, and disrupts optimal protein synthesis and mitochondrial energy production. This hastens functional decline reflected in heightened risk factors for numerous chronic diseases and co-occurring health issues earlier in life such as cancer, diabetes, heart disease, liver conditions, stroke, and cognitive and mental health disorders indicative of brain shrinking with atrophy.
Booze also withers connections between neurons, shrinking brain volume integrity–thus progressively damaging the speed and accuracy of neurotransmission channels. Over the years, these systemic degenerative cascades profoundly degrade the body’s intrinsic repair mechanisms, speed susceptibility to disorders, and present a biological age that far surpasses chronological age.
Prolonged heavy alcohol consumption definitively dulls executive functions and intelligence—including attentional focus, planning, organizational capabilities, and cognitive flexibility, as well as memory formation and recall capacities mediated by the prefrontal, temporal, and hippocampal regions. Shrinking brain volume via substance-driven cerebral atrophy, neural inflammation, and hampered neuroplasticity compound cumulative losses in processing speed, reasoning, and verbal fluency. This reflects pathology patterns implicated in frontotemporal dementia, illustrating potential severity levels.
Alcohol severely disrupts delicate neurotransmitter equilibrium maintaining a stable disposition, and can cause significant neurochemical and hormonal volatility. This explains the heavy mood swings that can occur the day after a night of drinking.
The intertwined cycles of rising and crashing signals of key molecules like serotonin, dopamine, cortisol, GABA, and glutamate alongside sensitization of the limbic amygdala generate internal biopsychosocial chaos. This compounds pre-existing psychiatric symptoms and risk factors for new mood disorders amid challenges regulating emotional reactivity. Mood may ricochet from feelings of despair one moment to aggressive irritation the next – especially amid low social support.
Even moderate intoxication impedes neural connectivity between the prefrontal executive control centers. These areas of the brain, like the amygdala and basal ganglia, are responsible for emotional processing and are affected by alcohol –thus sabotaging finely tuned communication pathways that govern behavior.
This in turn spurs a “Jekyll and Hyde” behavioral disinhibition, wherein suppression of inherent constraints against violence, crime, inappropriate sexualization, aggression, and reckless thrill-seeking lifts, contravening ingrained morals. Individuals may act in atypically dangerous, destructive ways fueled by alcohol inhibition of neural networks regulating judgment, farsightedness, and discretion that control behavior.
Alcohol misuse can severely impact the liver over time due to the hepatotoxic inflammatory stress caused by metabolizing excessive amounts of alcohol. This can lead to fatty liver, alcoholic hepatitis, chronic liver disease, and cirrhosis. The oxidative stress alcohol places on liver cells impairs their ability to manage toxins and waste, while also scarring tissue. This escalates risk factors for complications like hepatic encephalopathy, fluid retention, and eventually liver cancer or failure.
While environmental factors influence drinking habits, there are also underlying genetic links that may predispose someone to developing AUD. Certain gene variants regulating alcohol metabolism rates as well as the neurotransmitter systems governing mood, judgment, and impulse control seem to escalate biological risk levels.
Petrakis, I. L. (2002). Comorbidity of Alcoholism and Psychiatric Disorders: An Overview. PubMed Central (PMC). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6683830/
Kessler, R. C., Nelson, C. P., McGonagle, K. A., Edlund, J., Frank, R. G., & Leaf, P. J. (1996, January 1). The epidemiology of co-occurring addictive and mental disorders: Implications for prevention and service utilization. American Journal of Orthopsychiatry. https://doi.org/10.1037/h0080151
Comorbidity of mental disorders with alcohol and other drug abuse. Results from the Epidemiologic Catchment Area (ECA) Study. (1990, November 21). PubMed. https://pubmed.ncbi.nlm.nih.gov/2232018/
Dharavath, R. N., Pina-Leblanc, C., Tang, V. M., Sloan, M. E., Nikolova, Y. S., Pangarov, P., Ruocco, A. C., Shield, K. D., Voineskos, D., Blumberger, D. M., Boileau, I., Bozinoff, N., Gerretsen, P., Vieira, R. L. M., Melamed, O. C., Sibille, E., Quilty, L. C., & Prevot, T. D. (2023, October 20). GABAergic signaling in alcohol use disorder and withdrawal: pathological involvement and therapeutic potential. Frontiers in Neural Circuits. https://doi.org/10.3389/fncir.2023.1218737
Di Chiara, G. (1997). Alcohol and Dopamine. PubMed Central (PMC). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6826820/
Banerjee, N. (2014, January 1). Neurotransmitters in alcoholism: A review of neurobiological and genetic studies. Indian Journal of Human Genetics. https://doi.org/10.4103/0971-6866.132750
Kumar, S., Porcu, P., Werner, D. F., Matthews, D. B., Diaz-Granados, J. L., Helfand, R. S., & Morrow, A. L. (2009). The role of GABAA receptors in the chronic and short-term effects of ethanol: A decade of progress. Psychopharmacology, 205(4), 529. https://doi.org/10.1007/s00213-009-1562-z
Daviet, R., Aydogan, G., Jagannathan, K., Spilka, N., Koellinger, P., Kranzler, H. R., Nave, G., & Wetherill, R. R. (2022, March 4). Associations between alcohol consumption and gray and white matter volumes in the UK Biobank. Nature Communications. https://doi.org/10.1038/s41467-022-28735-5
Kubota, M., Nakazaki, S., Hirai, S., Saeki, N., Yamaura, A., & Kusaka, T. (2001, July 1). Alcohol consumption and frontal lobe shrinkage: a study of 1432 non-alcoholic subjects. Journal of Neurology, Neurosurgery, and Psychiatry. https://doi.org/10.1136/jnnp.71.1.104
Staples, M. C., & Mandyam, C. D. (2016, September 30). Thinking after Drinking: Impaired Hippocampal-Dependent Cognition in Human Alcoholics and Animal Models of Alcohol Dependence. Frontiers in Psychiatry. https://doi.org/10.3389/fpsyt.2016.00162
Alcohol Use Disorder: From Risk to Diagnosis to Recovery | National Institute on Alcohol Abuse and Alcoholism (NIAAA). (2023, September 22). https://www.niaaa.nih.gov/health-professionals-communities/core-resource-on-alcohol/alcohol-use-disorder-risk-diagnosis-recovery
Hasin, D. S., Stinson, F. S., Ogburn, E. L., & Grant, B. F. (2007, July 1). Prevalence, Correlates, Disability, and Comorbidity of DSM-IV Alcohol Abuse and Dependence in the United States. Archives of General Psychiatry. https://doi.org/10.1001/archpsyc.64.7.830
Are mental health and poverty connected?
Can yoga help with mental illness?
10 habits to improve mental health
What are the stages of alcohol addiction?
What are the statistics of alcohol abuse in the United States?